Pulse oximetry is a type of test that uses a pulse oximeter to measure oxygen levels in the blood.
Healthcare providers use this test to assess how well oxygen is being transported throughout the body and if a person is experiencing hypoxemia, or below normal levels of oxygen in the blood.
Table of Contents
What is oxygen saturation?
To understand pulse oximetry, we must first understand oxygen saturation (often abbreviated as O2sat or SaO2).
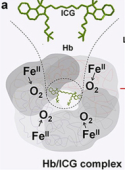
Red blood cells contain hemoglobin, and a single molecule of hemoglobin in the blood can carry four oxygen molecules.
When oxygen is bound to hemoglobin, the hemoglobin molecule is considered to be “saturated” with oxygen.
If all four binding sites on a hemoglobin molecule are carrying oxygen, this is described as an oxygen saturation of 100%.
In other words, oxygen saturation is a percentage of how much oxygen the blood is carrying out of the maximum amount of oxygen that is able to be carried in the blood.
In a healthy individual, oxygen saturation is 95-100%. According to the World Health Organization (WHO), when oxygen saturation drops below 90%, this is considered to be a clinical emergency.
What does a pulse oximeter measure?
To conduct pulse oximetry, a small device called a pulse oximeter, or pulse ox, is used to measure oxygen levels.
Specifically, a pulse oximeter measures:
- Oxygen saturation: since pulse oximeters typically obtain readings peripherally at the finger, toe, or ear, the result is referred to as the peripheral oxygen saturation (or SpO2)
- Pulse rate: also referred to as the heart rate, this reading is an indicator of how well the tissues are perfused with blood and oxygen; pulse oximeters show pulse rate in beats per minute (bpm), and a normal pulse rate is 60-100 bpm
Pulse oximeters continuously measure oxygen saturation level and pulse rate and are therefore relied upon for providing early warnings of hypoxia (below normal levels of oxygen in the body) or hypoxemia.
What happens when oxygen saturation is low?
When oxygen saturation is below normal (ie, hypoxemia), a range of symptoms can occur, depending on the severity of the condition:
- Shortness of breath
- Fast heartbeat
- Coughing
- Wheezing
- Headache
- Confusion
- Blueish color in lips, skin, and fingernails
Insufficient oxygen in the blood can lead to damage in the heart and brain, making monitoring oxygen saturation with methods such as pulse oximetry extremely important.
What is pulse oximetry used for?
There are quite a few situations where a healthcare practitioner would need to know if a person has sufficient levels of oxygen in the blood:
- To check if a person intermittently stops breathing during sleep (ie, sleep apnea)
- During or after surgery or medical procedures that require sedation
- To assess a person’s ability to handle increased physical activity
- To assess how well lung medications are working
- To see how well a ventilator is working or if it is needed
Furthermore, pulse oximetry is also used with medical conditions that affect blood oxygen levels, such as:
- Asthma
- Chronic obstructive pulmonary disorder (CODP)
- Heart failure
- Heart attack
- Pneumonia
- Lung cancer
- Anemia
What are the risks of pulse oximetry?
Pulse oximeters are easy to use and are painless, as they don’t require any needles. However, a main concern with pulse oximeters is receiving incorrect readings if the pulse oximeter falls off.
Risks can vary depending on a person’s general health and other comorbid conditions. It is always good to speak with a healthcare practitioner about any other concerns.
How do pulse oximeters work?
One of the most common types of pulse oximeters is designed as a clip that attaches to the finger, toe, or earlobe.
These pulse oximeters emit beams of light that pass through the blood at the finger, toe, or earlobe to measure oxygen saturation.
Readings are obtained by detecting changes in light absorption that occur depending on the level of oxygen saturation in the blood. Pulse oximeters also provide heart rate (or pulse) readings simultaneously.
What is the Best Finger Pulse Oximeter? (Reviews and Buying Guide)
References
- World Health Organization. Pulse Oximetry Training Manual. https://www.who.int/patientsafety/safesurgery/pulse_oximetry/who_ps_pulse_oxymetry_training_manual_en.pdf. Published 2011. Accessed June 2022.
- Johns Hopkins Medicine. Pulse Oximetry. https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/pulse-oximetry. Accessed June 2022.
- American Thoracic Society. Pulse Oximetry. https://www.thoracic.org/patients/patient-resources/resources/pulse-oximetry.pdf. Updated March 2018. Accessed June 2022.
- American Lung Association. Pulse Oximetry. https://www.lung.org/lung-health-diseases/lung-procedures-and-tests/pulse-oximetry. Updated May 2022. Accessed June 2022.
- Cleveland Clinic. Hypoxemia. https://my.clevelandclinic.org/health/diseases/17727-hypoxemia. Reviewed March 2018. Accessed June 2022.
- University of Iowa Healthcare. Pulse Oximetry Basic Principles and Interpretation. https://medicine.uiowa.edu/iowaprotocols/pulse-oximetry-basic-principles-and-interpretation. Modified October 2017. Accessed June 2022.
Images courtesy of Visual Hunt and Open Access Biomedical Image Search Engine.